
We examine federal requirements and guidance on who can be charged for COVID-19 testing and related services. 
Some patients may be billed for testing-related care from the hospital, a provider, or the insurer. These services are required to be covered by insurance nonetheless patients may experience problems with billing or claims denials. We were able to find COVID-19 diagnostic test prices for 93 out of 102 hospitals, ranging from $20 – $1,419 per single test, not including the price of a provider visit, facility fee, or specimen collection. For each state, we searched for COVID-19 test prices posted on public websites of the two largest hospitals. In this brief, we present the findings from our search for COVID-19 test prices, which we conducted from April 20 through April 27, 2021. However, the CARES Act price transparency rule provides a unique opportunity to examine what insurers pay for out-of-network care that is required to be covered. Negotiated rates (between payers and their in-network providers for COVID-19 testing) are not always publicly available. Health & Wellbeing Premature mortality during COVID-19 in the U.S. 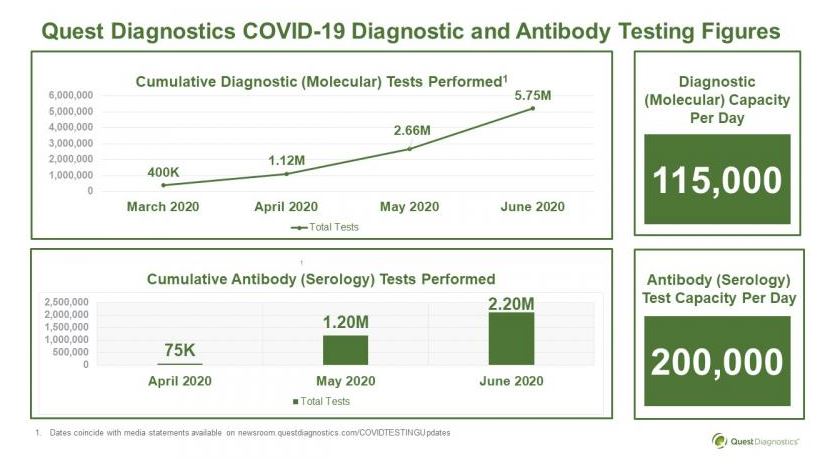
These CARES Act coverage and payment requirements apply during the duration of the public health emergency. The CARES Act requires providers to post the cash price on their public website for insurer use. In the absence of a negotiated rate for out-of-network providers, insurers must pay the provider’s cash price – sometimes called the list price – for COVID-19 testing and related services. 
Private health insurers negotiate allowed charges with hospitals and providers participating in their network. Much like for other health services, hospitals and laboratories can set their own rates for privately insured and uninsured individuals. Outside of the Medicare program, there is no federal regulation of the price of COVID-19 diagnostic tests or other related tests and visits. Such limits mean some patients with health coverage may nonetheless receive bills for COVID-19 diagnostic testing and related services, and those bills often can be widely different from patient to patient. However, insurers are not required to cover COVID-19 testing without cost-sharing if it is conducted as part of employee return-to-work programs or public health surveillance purposes. Some denied COVID-19 testing claims unless directly ordered by a physician.įederal guidance released in early 2021 under the Biden Administration clarified that insurers must cover testing without cost sharing for asymptomatic individuals and without requiring medical screenings. For example, some plans denied COVID-19 testing claims or applied cost sharing for COVID-19 testing for asymptomatic individuals unless they had known or suspected exposed to COVID-19 and had a referral for testing from their provider. Since enactment, questions have arisen about the scope of protections and when they apply. Federal laws also made resources available to finance free testing for uninsured individuals. Two major legislative efforts passed at the onset of the pandemic in March 2020 – the Families First Coronavirus Response Act ( FFCRA) and the Coronavirus Aid, Relief, and Economic Security (CARES) Act – required health coverage for COVID-19 testing – including the test itself, the related visit, and other services related to testing – with no cost-sharing for people covered by most private health plans, Medicare, and Medicaid. NOTE: This analysis was updated in April, 2021.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
